This article was first published by Oliver Wyman here.
Editor’s note: This is part of an ongoing series on how pharmaceutical companies can impact and help reduce health inequities.
Among the issues confronting healthcare leaders perhaps none presents more challenges or opportunities than health equity. The complexity of the problem cuts across age, ethnicity, gender, and race. And it’s both an outcomes and access problem. The statistics tell the story:
- Hispanic patients are 50% more likely to die from diabetes than white patients
- Black patients are 25% less likely to be discharged from the hospital on a direct-acting oral anticoagulant than white patients
- Women have a 20% higher chance of developing heart failure or dying within five years of their first heart attack than men
- People aged 70 years or older account for 42% of cancer patients but just 25% of clinical trial participants
While health equity is largely viewed as the domain of governments, providers, and payers, pharmaceutical companies can — and must — play a role in closing gaps in medical access and outcomes. In fact, pharmaceutical companies are uniquely positioned to help reduce health disparities. From drug development and clinical trials to medication adherence, pharmaceutical companies have a reach that cuts across the entire health ecosystem and patient journey. While the sector has targeted disparities globally, the COVID-19 pandemic put a spotlight on prominent vulnerabilities in developed nations. To have an impact, health equity must become a priority as both a moral and business imperative – with commitments by corporate leaders to engrain health equity within the product life cycle.
ROOT CAUSES
A myriad of issues has led to the proliferation of health inequities. Some are deeply rooted within the healthcare delivery system; others are social determinants that require action by a broader set of stakeholders. In thinking about the pharmaceutical industry, we homed in on three categories:
- Limited medical knowledge: Essential to understanding how to treat patient populations is knowing what to look for. Unfortunately, women and non-white populations are disproportionately understudied and underrepresented in clinical trials. In 2020, the US Food and Drug Administration found that 75% of patients involved clinical trials were white. By comparison, 6% were Asian, 8% were Black, and 11% were Hispanic. Just 30% of participants were 65 years of age or older. And researchers at Brigham and Women’s Hospital reported that women account for 41% of clinical trial participants; the figure drops to 22% when considering Phase I trials, according to US government data. As we strive toward personalized medicine, we need to get ahead of our gaps and broaden the diversity of mapped genomes. Currently, ~78% of the people in genome-wide association studies are of European descent, even though they only account of 16% of the global population.
- Bias at the bedside: Conscious or unconscious, bias creeps into clinical decision-making. This impacts what tests patients are given, how they are treated, and, eventually, their outcomes. Some biases are institutional and have been in place for decades — the Institute of Medicine’s landmark 2003 report Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care noted that Blacks and Hispanics are less likely than whites to receive such cardiac medications, even after social determinants of health are considered. Personal biases also have an impact. For instance, 40% of first- and second-year medical students endorsed the notion Black people’s skin is “thicker” than white people’s skin, which leads to biases in how pain is assessed and treated. And the lack of medical knowledge outlined in the previous bullet contributes to biases. Further illustrating the point, a recent JAMA Network study highlighted the challenge US health systems face in developing population health strategies for underserved groups due to a dearth of family history information. But bias works both ways due to long-standing trust issues patients have with the healthcare industry. That lack of trust leads to patients disregarding clinical information and treatment protocols. Speakers at last month’s Oliver Wyman Health Innovation Summit detailed ramifications that eroding trust has on the industry and patients.
- Social barriers: Where you were born or live is often a strong predictor of their medical history. Such social determinants as housing, food and nutrition, transportation, and employment status can affect 50% of health outcomes (some studies place it as high as 80%). People born in high human development countries live 19 years longer than those born in low human development countries. Researchers have also found a correlation between social determinants of health and the onset of chronic disease.
Gaps in these and other areas lead to a range of challenges in the patient journey (Editor's note - click on a box to see supporting statistics):
AN IMPERATIVE FOR PHARMA
Pharmaceutical companies can expand the industry’s base of knowledge by building more age, ethnicity, gender, and racial diversity into the product life cycle. In doing so, they can propel care towards more personalized medicine. But for this to happen, executives and boards of directors need to make health equity a priority at the corporate level. As the Institute for Healthcare Improvement noted when talking about health equity in the provider space, “senior management must not only articulate the vision, but also act on it by building it into all high-level decision-making. That direction-setting from the top puts the strategy directly into practice and sets the tone for the entire organization.” The same philosophy applies to pharmaceutical companies.
Once elevated to the corporate level, health equity can be incorporated across the life cycle of pharma products. That means breaking down barriers and silos that exist between functions. A product’s go-to-market strategy will fail if medical, marketing, access and sales teams are not on the same page. For example, by tapping into analytics, companies can gain a detailed understanding of variations in treatment patterns. That data can then be shared with providers to develop more appropriate protocols. The point is pharmaceutical companies can influence the patient journey in a variety of ways and across a variety of settings:
PHARMACEUTICAL COMPANIES CAN DISRUPT SYSTEMIC BARRIERS TO HEALTH EQUITY
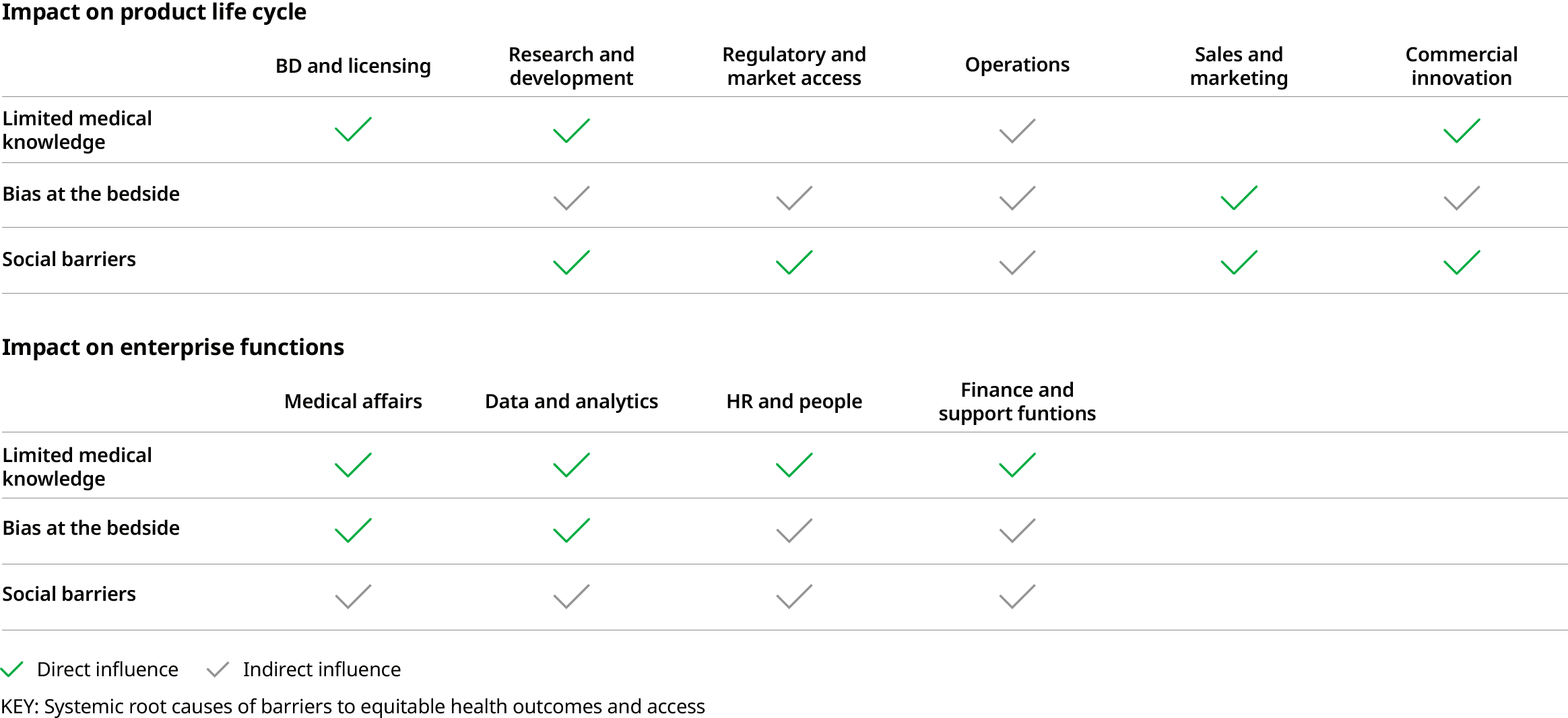

FOCUSING ON OUTCOMES
Those achieving transformative impact have developed an enterprise strategy with measurable goals. To create meaningful value, organizations need to align and focus on what challenges to tackle and how. Oliver Wyman’s approach starts with confirming – or creating as needed – senior alignment on the organization’s broader health equity vision. This shared understanding serves as key guidance to strategy development, particularly when determining:
1. Where to look to identify disparities that the organization can address
2. Which disparities to assess root causes as areas of “first focus” (typically hyper-local, and not easily generalizable across underrepresented groups)
3. What types of effective interventions to implement (also typically hyper-local, requiring heavy coordination with local organizations)
Given the hyper-locality of both root-causes for disparity and effective interventions available within communities to address these root causes, it is critical to develop re-useable frameworks, tools, and approaches, often bespoke to specific organization’s product development cycle, to enable scaling of health equity strategies beyond specific therapeutic areas. We ensure the teams we work with while developing these strategies and supporting roadmaps are familiar and comfortable with using these assets in other parts of the organization.
MODELING SUCCESS: CASE STUDIES
Getting pharmaceutical companies to take on such a heady issue health equity is not a hypothetical. We’ve seen pockets of success playout in different ways. Leaders from Merck told us how they were able to move the needle on diabetes care by identifying commonalities among populations that were being diagnosed in later stages of the disease. Through a comprehensive data project, they developed a robust understanding of the patient journey and created culturally and locally relevant outreach and screening campaigns. The result was more patients being diagnosed at an earlier state, allowing clinicians to develop a disease management plan more effectively.
As another example, we worked with a Pharma client to develop strategies to overcome barriers to treatment faced by underserved populations. Our assessment mapped underserved populations — rural and remote communities, uninsured, immigrants, refugees, low income, minority pops, low HC understanding, low education status, limited social embedding (those who live in relative isolation) — across multiple root causes which centered around ‘location’, ‘income’, ‘awareness’, and ‘community.’
Leveraging commonalities where possible, we identified methods for improving access specific to our client’s capabilities and areas of influence – examples include: digital tools to both educate clinicians and improve connectivity with relevant specialists, artificial intelligence to aid accurate diagnosis outside of specialist centres, “at home” patient engagement, fixed cost/discounted transportation (e.g., in partnership with ride-sharing companies), patient awareness campaigns, and financial programs aimed at improving patient affordability. These solutions could then be incorporated across countries based on their own assessment and prioritization of root causes impacting access.
So, what’s next? This is a pivotal moment for the industry. The COVID-19 pandemic put a bright spotlight on how inequities have an oversized impact on patient outcomes across the globe and put developed countries under a microscope. Pharmaceutical companies not only have an opportunity, but an obligation, to drive solutions. And as leaders assess their organization’s position, a key question to ask is this: How should health equity stand on its own as a corporate priority while also driving environmental, social, and governance mission? We’ll explore that, and other topics, in upcoming articles in this series.
James Hooton, Engagement Manager, Oliver Wyman, contributed to this article.
To learn more contact Matthew Weinstock, Senior Editor, Health and Life Sciences.